Differences between Crohn’s disease and ulcerative colitis
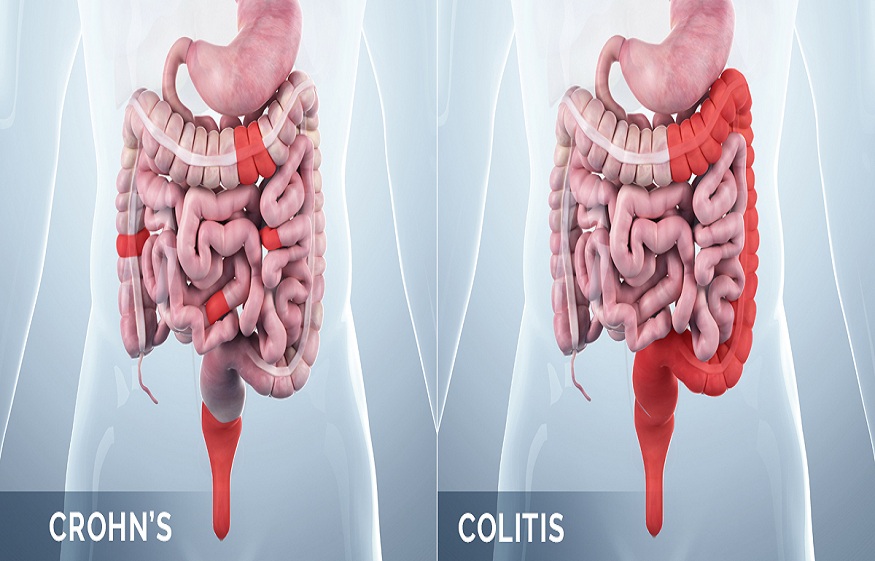
Although Crohn’s disease and ulcerative colitis may seem the same, the truth is that each of them has its peculiarities, although it is true that they share many aspects. Among them, the mechanism of the inflammatory process, which is the same in both ailments.
In addition, both are part of what is called Inflammatory Bowel Diseases. The most characteristic symptoms are quite similar in the two conditions, although their affect areas are different.
Among their differences are also the injuries they cause. For example, Crohn’s disease preferentially damages the small intestine. It can lead to granulomas (spherical masses made up of cells of the immune system that clump together when trying to isolate substances that the body does not recognize) and fistulas (fissures that open on the skin or mucous membranes). On the other hand, ulcerative colitis does not injure the small intestine or cause granulomas or fistulas.
This is because, in Crohn’s disease, inflammation penetrates the entire intestinal wall, making it thickened, whereas ulcerative colitis only affects the deepest part of the intestinal wall.
Another difference between ulcerative colitis and Crohn’s is that the latter can leave common areas between the areas affected by inflammation, which does not occur in ulcerative colitis.
Diet in Crohn’s disease
The problem of malnutrition
It is relatively common for people with Crohn’s disease to have nutritional deficiencies, which is somewhat logical since it affects the digestive tract. Therefore, if you suffer from this disease, you must take care of your diet to ensure that you receive all the nutrients that your body needs. Because malnutrition, contrary to what you may think, does not have to affect only thin people. For example, 35% of patients with Crohn’s disease in remission are overweight, and up to 10% are obese. And despite this, many of these patients lack nutrients such as vitamins and minerals.
.This is due to various factors. One of the most important is that when patients are unwell due to flare-ups, they eat less because they have less appetite. It may also happen that they avoid eating because doing so causes symptoms. If in your case, this is not the problem and you have a deficiency of some vitamins or minerals, it could be that the inflammation of the small intestine causes worse assimilation of food.
The most common symptoms of the disease, such as diarrhea, also do not help retain protein, iron, or salts. Also, the surgery involving the removal of part of the small intestine can be why some vitamins, such as B12, are not assimilated well.
But why is it essential to prevent this nutritional deficit? If we do not give our body everything it needs to function, the consequence can be, in addition to weight loss, other complications such as anemia, decalcification of the bones, or growth retardation in children and adolescents. Hence the importance of taking care of this aspect from the moment the disease is diagnosed.
As a Crohn’s patient, you have a greater chance of having some nutritional deficits, it is convenient that you take care of your diet and values with your doctor or nutritionist for a suitable diet for you. The goal is to prevent malnutrition or correct it if it has already occurred.
Take care of the diet.
Everything you eat has a positive or negative impact on your body. If, you do not eat all the necessary nutrients and inadequate amounts for whatever reason (food assimilation problems, lack of appetite, etc), this can affect your health.
In principle, the diet you follow should be as varied as possible. Proteins, calcium, and iron are some of the components that you should take into account the most when thinking about your daily menu. Proteins can be obtained from eggs, meat, fish, legumes, and milk and its derivatives. The latter will also provide calcium for the bones. Iron, also essential in your diet, is found mainly in red meat, liver, legumes, cereals, and nuts.
Should you avoid any food?
Surely you have wondered if there is any food that you should avoid or something that worsens Crohn’s disease’s inflammation and, therefore, you should limit its intake. No single food has been shown to trigger outbreaks of Crohn’s disease or make the condition worse. You should only avoid those foods that you identify that make your symptoms worse.
This should be checked more than once, because sometimes you can feel bad after eating some food and think that it is because of it, when it may be because your body does not feel well, regardless of what you have eaten at that time. In this way, you will avoid doing without foods that do not cause you any harm and that could provide you with many nutrients.
Fiber consumption
One of the foods that Crohn’s patients often wonder if they can eat is fiber. It is essential to differentiate between insoluble fiber (which produces much fecal waste) and soluble fiber (which produces less waste).
If you suffer from intestinal strictures (strictures) due to your disease, you should avoid anything that facilitates intestinal obstruction or damage the mucosa of the small intestine and colon. And this can happen with insoluble fiber. Therefore, if you are in an outbreak period of your disease and have intestinal strictures, avoid this type of fiber you can find in whole foods, in cereal preparations, bran, and some vegetables such as asparagus, artichokes, or legumes.
On the other hand, dairy consumption is not related to Crohn’s disease’s origin or worsening. Indeed, the body of some people may not be able to assimilate lactose but, in this case, lactose intolerance is independent of the fact of having Crohn’s disease.
What is artificial nutrition?
Sometimes the malnutrition that a person with Crohn’s disease may suffer from can be severe and, in these cases, the diet may not be enough to correct this situation. It is at these times that it can be useful to resort to artificial nutrition, of which there are two types:
- Parenteral nutrition: In this type of nutrition, the intravenous route is used to administer nutrients directly to the blood.
- Enteral nutrition: It is the most used. It is taken by mouth, although sometimes it can also be administered directly to the stomach through a tube.